Artificial Intelligence–Enabled ECG for Early Detection of Structural Heart Disease: Clinical Evidence, Applications, and Limitations
Artificial Intelligence–Enabled ECG for Early Detection of Structural Heart Disease: Clinical Evidence, Applications, and Limitations
Introduction
Cardiovascular disease remains the leading cause of mortality worldwide, accounting for nearly 20 million deaths annually. A major contributor to this burden is structural heart disease (SHD)—including left ventricular systolic dysfunction (LVSD), hypertrophic cardiomyopathy, valvular disease, and cardiomyopathies—which often progresses silently before symptoms emerge.
Traditional diagnostic pathways rely heavily on imaging modalities such as echocardiography and cardiac MRI. While effective, these tools are resource-intensive and not scalable for population-wide screening. In contrast, the electrocardiogram (ECG) is inexpensive, ubiquitous, and standardized globally.
Recent advances in artificial intelligence (AI)—particularly deep learning—have transformed the ECG from a simple electrical tracing into a high-dimensional predictive biomarker capable of identifying structural abnormalities that are not visually apparent to clinicians. This article reviews the scientific basis, clinical validation, implementation landscape, and limitations of AI-enabled ECG models for structural heart disease detection.
The Scientific Foundation of AI-Enabled ECG Interpretation
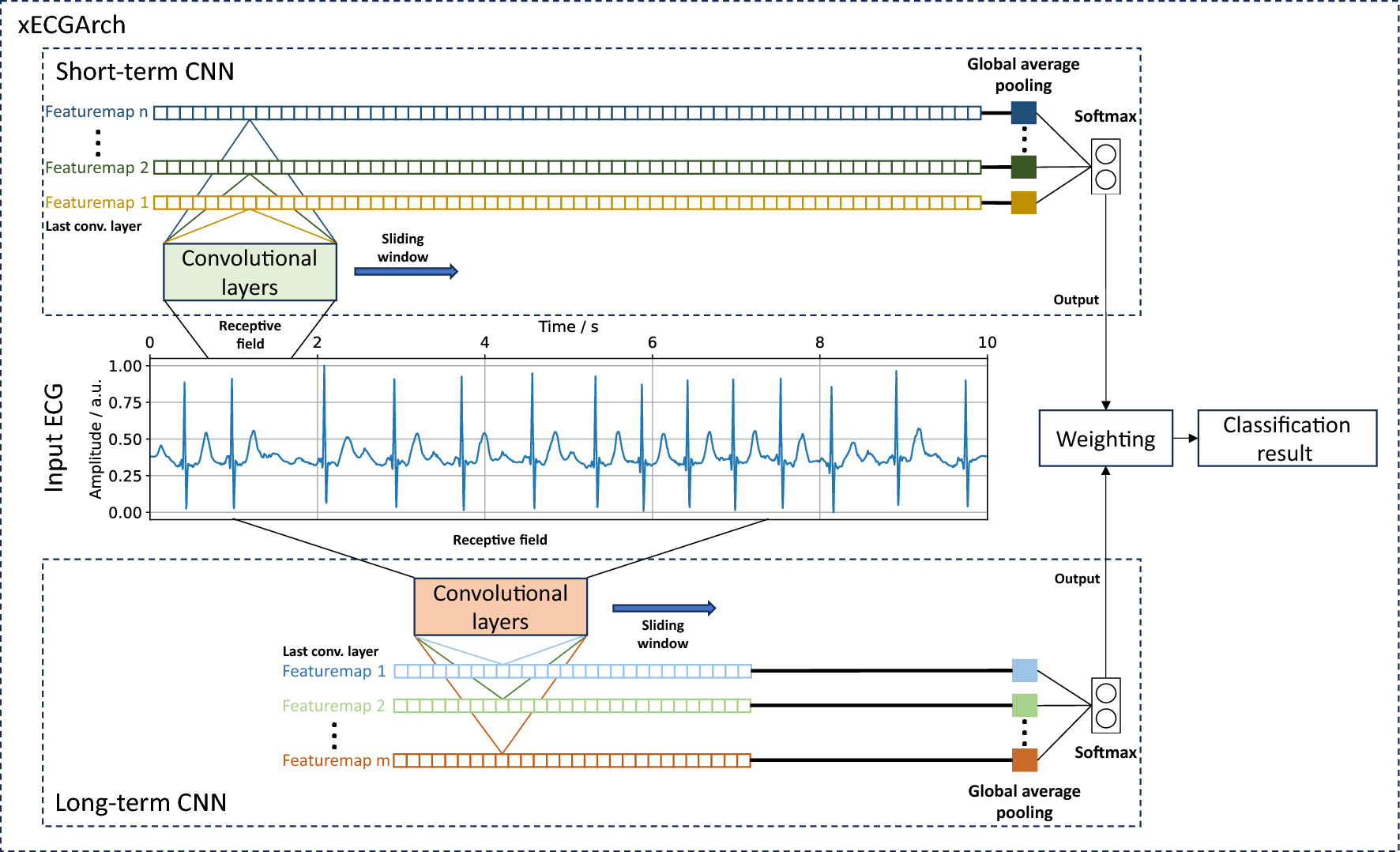
Traditional ECG interpretation is based on recognizable waveform patterns. However, modern deep learning models—particularly convolutional neural networks (CNNs)—analyze raw waveform data to identify complex, nonlinear relationships that exceed human perceptual capacity.
A landmark study from Mayo Clinic demonstrated that a deep neural network trained on over 44,000 ECGs could identify asymptomatic left ventricular dysfunction with an area under the curve (AUC) of 0.93 (Attia et al., 2019). Importantly, many of these patients had normal ECG readings by conventional standards.
This marked a paradigm shift: the ECG could now function as a screening tool for structural abnormalities traditionally requiring imaging.
Key Clinical Applications
1. Detection of Left Ventricular Systolic Dysfunction (LVSD)

LVSD is a leading precursor to heart failure. Early detection dramatically improves outcomes through timely initiation of guideline-directed medical therapy.
Two pivotal studies illustrate the clinical relevance:
Attia et al., 2019 (Nature Medicine)
Deep learning model trained on 44,959 patients
AUC = 0.93 for detecting EF ≤35%
Citation: Attia ZI et al. Nature Medicine. 2019;25:70–74.Prospective Validation Study (Mayo Clinic, 2022)
Real-world deployment showed that AI-flagged patients were more likely to be diagnosed with previously unrecognized LVSD within follow-up periods.
Citation: Attia ZI et al. The Lancet Digital Health. 2022;4:e333–e341.
Implication: AI-ECG models can identify high-risk patients before overt clinical deterioration.
2. Screening for Hypertrophic Cardiomyopathy (HCM)

Hypertrophic cardiomyopathy often presents with subtle ECG changes and may remain undiagnosed until severe events occur.
A study by Ko et al. (2020) demonstrated that AI-based ECG analysis could detect HCM with high sensitivity, outperforming traditional rule-based criteria.
Citation: Ko WY et al. Nature Medicine. 2020;26:1–8.
Clinical relevance: Population-scale screening may become feasible without universal echocardiography.
3. Prediction of Future Atrial Fibrillation
AI-ECG models have also shown the ability to predict future atrial fibrillation (AF) even when patients are in sinus rhythm.
Attia et al., 2019 (Circulation)
AI model predicted future AF with AUC 0.87.
Citation: Attia ZI et al. Circulation. 2019;140:1287–1298.
This demonstrates that ECG signals contain latent predictive information beyond visible arrhythmias.
Implementation in Clinical Practice
AI-ECG systems are being integrated into electronic health records and hospital workflows in academic centers. Regulatory pathways have also advanced, with multiple AI-based cardiology tools receiving FDA clearance.
However, translation from controlled research settings to heterogeneous populations remains ongoing.
Two implementation realities:
Performance may decline in diverse or underrepresented populations.
Clinical integration requires workflow redesign and clinician education.
Strengths of AI-Enabled ECG Screening
Scalability – ECG machines are already present in primary care and rural settings.
Cost Efficiency – No additional imaging required for initial screening.
Automation – Minimal added clinician burden once integrated.
Population Health Potential – Enables proactive, not reactive, cardiology.
Limitations and Critical Appraisal
Despite strong performance metrics, several challenges remain:
1. External Validity
Many models are trained on single-center datasets. Generalizability across ethnic, geographic, and socioeconomic groups requires broader validation.
2. Algorithmic Bias
Underrepresentation of minority populations in training datasets risks reduced diagnostic accuracy in vulnerable groups.
3. Interpretability
While performance is high, mechanistic understanding of what waveform features drive predictions remains limited.
4. Overdiagnosis Risk
High-sensitivity models may increase downstream imaging and healthcare costs if not implemented judiciously.
Future Directions
The next phase of AI-ECG development is likely to include:
Federated learning across multinational datasets
Integration with wearable ECG devices
Multimodal fusion (ECG + imaging + biomarkers)
Continuous monitoring platforms
Large-scale pragmatic trials will determine whether AI-ECG screening reduces mortality and hospitalization at the population level.
Conclusion
Artificial intelligence–enabled ECG analysis represents one of the most clinically validated and scalable applications of AI in cardiology. By extracting latent predictive information from routine ECG recordings, deep learning models can detect structural heart disease before symptoms arise.
However, widespread adoption must proceed with rigorous external validation, careful attention to bias, and integration into evidence-based care pathways.
The ECG is no longer just a diagnostic tracing—it is emerging as a computational biomarker platform with transformative potential in cardiovascular medicine.
References
Attia ZI et al. Screening for cardiac dysfunction using artificial intelligence–enabled ECG. Nature Medicine. 2019;25:70–74.
Attia ZI et al. Prospective validation of AI-enabled ECG. The Lancet Digital Health. 2022;4:e333–e341.
Ko WY et al. Detection of hypertrophic cardiomyopathy using AI-ECG. Nature Medicine. 2020;26:1–8.
Attia ZI et al. AI-enabled prediction of atrial fibrillation. Circulation. 2019;140:1287–1298.
World Health Organization. Global cardiovascular disease statistics, 2023.


Comments
Post a Comment